AIDS Patient Care and STDs, Volume 13, Issue 12, Pages 709-716. December 1999.
AIDS Patient Care and STDs, Volume 13, Issue 12, Pages 709-716. December 1999.
There are over 100 million girls and women who have undergone female genital mutilation (FGM). The World Health Organization (WHO) estimates that another 2 million are subject to it every year. FGM is practiced in many countries, especially Africa and parts of the Middle East. Various degrees of FGM are prevalent, the most mutilating one being infibulation (pharaonic). With infibulation there are numerous life-long health problems such as hemorrhage, infection, dyspareunia, genital ulcers, and gynecological and obstetrical complications. It has been postulated that FGM may also play a significant role in facilitating the transmission of HIV infection through numerous mechanisms. In this article several of the most common complications are discussed and helpful suggestions for management during pregnancy and delivery are explored.Included are the legal and ethical ramifications.
FEMALE GENITAL MUTILATION (FGM), which is inaccurately referred to as female circumcision by some people, has been practiced for centuries. Egyptian mummies were found to have been circumcised as far back as 200 B. C. In the 19th Century it was practiced in Europe and North America as a remedy for ailments like epilepsy, hysteria, and masturbation.1 The practice of FGM is most prevalent in the African countries such as Nigeria, Ethiopia, Sudan, Egypt, and some area of the Middle East. It is not restricted to any ethnic, religious or socioeconomic class. There are many reasons for perpetuation of this practice, the most common are cultural and religious beliefs. Although often associated with Islam, it is also practiced by other religious groups, including Christians. There is no mention of it in the Koran. An overwhelming factor for its justification is the cultural influence and traditions, social acceptance within the community, and ensuring chastity and fidelity by attenuating sexual desire.2,3 A research study done in Nigeria on the Igbos tribe found that women believe that FGM makes them more feminine and thus more attractive to men.4 A recent social study carried out established that FGM raises the social status for the family and generates income when the daughter gets married and thedowry is paid.5
The World Health Organization (WHO), in an effort to standardize the terminology has divided FGM into four main groups. Dr. Naid Toubia, who has researched and written extensively on this topic, has identified two types. He combines type I and II and divides infibulation into type III and IV.6 This is not the case with WHO. For the purposes of this article, the WHOclinical classifications will be followed.
WHO has indentified a new category type IV, which encompasses other types of operations such as gihiri cut, piercing, cauterization, and insertion of corrosive substances into the vagina. Of course, one must remember that FGM is carried out mainly in villages by lay people, with little knowledge of anatomy, so there often occurs a combination of all of these types. FGM is performed any time from birth to just before marriage, but most commonly done between the ages of 4 to 10 years.10
Complications following FGM, especially if the girl is infibulated, are common and many are well documented. These may be immediate or late. The major immediate complications are, of course, hemorrhage from the dorsal artery, shock and then infection, urinary retention and tetanus, which can lead to mortality.10-12
Some late and long-term complications seen are urinary incontinence, cysts, urogenital tract infections, severe dyspareunia, pelvic inflammatory disease, infertility, and obstetrical problems such as delayed or obstructed second stage labor, trauma, and hemorrhage. Hemorrhage was also seen as a late complication especially in the newly married girl who was tightly infibulated and was subjected to forcible sex by the husband or who the husband defibulated using various instruments such as scissors, blades or knives.1,6,12,13
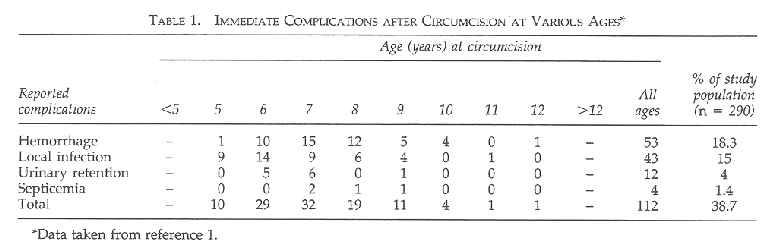
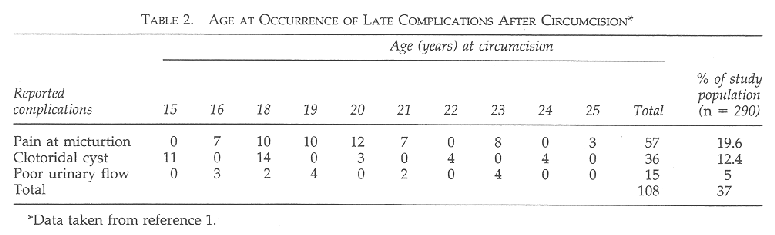
In the research done by Dirie and Lindmark in Somalia on 290 women (mean age 22 years, range 18 to 54), 88% of research subjects had excision and infibulation, the remainder fell into the less mutilating categories. Sixty-nine percent had this procedure performed at home and 52% of these were performed by an untrained person. The immediate main complication reported by 112 women in the study was hemorrhage, infection, urinary retention, and septicemia (see Table 1). Five women reported severe schock and two of them required blood transfusions. Those women with urinary retention were treated by splitting the infibulation scar and were reinfibulated a few weeks later. The late complication of which 108 women complained, were as follows: 36 with clitoral cysts, 29 requiring excision; 57 with pain on micturition; and 15 subjects had poor urinary flow (see Table 2).
Hemorrhage is an immediate as well as a late complication. For hemostasis the girl's legs are tied together and sometimes a poultice of crushed medicinal herbsis applied.4
The urinary retention reported by the women in the Dirie/Lindmark study occurred within the first 3 days after the operation and the reason given by the authors was that the girls tried to avoid passing urine because of the pain that urine causes when it irritates the raw surfaces. The retention was also due to skin flaps, blood clots or, in several cases the urinary meatus was sutured while closing the vulva.
Recurrent urinary tract infections and urinary problems were numerous, and according to Dirie/Lindmark, these were caused because the meatus was covered by the infibulation, causing vaginal dischange to accumulate and favor the growth of bacteria. The women reported that they were given antibiotics by their doctor and this helped.1 DeSilva14 reported that urinary tract infection with Escherichia coli was common in thesewomen.
The most common late complication of FGM that was reported by Dirie and several other authors was vulvar swelling, which was due to epidermal cyst formation that develops along the scar tissue and in the excised clitoral region. Hanly13 discusses 10 patients that attended the hospital in Tabuk, Saudia Arabia. All patients were immigrants into the Kingdom from Africa. Six patients presented with a large painless mass in the infibulation scar. Two complained of pain, one gave a history of a white continuous secretion for the scar site, and one complained of severe dyspareunia and had a cyst measuning 5.5 X 5 X % cm. The pathological finding in eight patients was of an implantation dermoid, in the other two patients the cyst had ruptured.
Mayad11 discusses the fibrous connective tissue tumors called fibromata. These form in the same areas as the dermoid cysts and also can grow to be large and pedunculated.
Pelvic inflammatory disease (PID), a common complication of sexually transmitted disease (STD) is accompanied by abdominal pain, infertility, and ectopic pregnancy. Research indicates that PID is a major problem worldwide and in some African countries, 22 to 44% of women admitted to the hospital for gynecological problems had PID. In women 20-29 years old, 7 to 25% of them were childless.15 The most prevalent organisms were Neisseria gonnorrhoeae and Chlamydia trachomatis. However, it is now believed that FGM plays a significant role in the development of PID. For the woman who has been infibulated there are added risks of infection and resulting infertility. It has been reported by Sami and El Dareer3 that chronic pelvic disease was three times more prevalent in the infibulated women. Chronic retention of unire, menstrual flow, and repeated urinary tract infections with E. coli are the consequences of poor drainage, which results from a space fromed behind the vulva skin. This then becomes an excellent reservoir for the growth of pathogenic organisms such as the E. coli.3,14,16
Shandall17 and DeSilva14 reported a high incidence of candiasis, which was more frequent with infibulation, and urine cultures showed the presence of mixed organisms, specifically E. coli. Shandall has suggested three main causes of PID in the infibulated woman, namely: (1) infection at the time of infibulation, (2) interference with drainage and (3) infection from spliting the infibulation and resulting resuture after labor. The infections then spread to the inner reproductive organs causing infertility.14,16,17
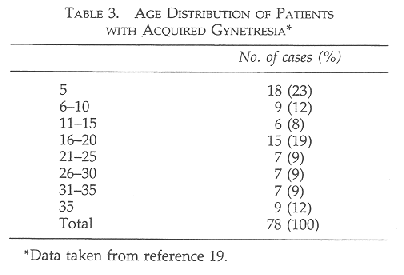
Rushwan states that FGM should be recognized as an important etiological factor for PID.18 Another reason for infertility is acquired gynetresia which according to Ozumba, is directly related to infibulation. In a study done by Ozumba in Eastern Nigeria on 78 women (see Tables 3 and 4), 59 patients (76%) had acquired gynetresia caused by infibulation. Sexual intercourse is generally difficult and the process of deinfibulation painful and can take 2-12 weeks to complete or even up to 2 years during which time the women seeks medical help for infertility.19

It is estimated that 2-25% of the cases of infertility in the Sudan are due to infibulation, either as a result of chronic pelvic infection or because of difficulty in having sexual intercourse and lack of penetration. In this society the psychological and social impact of being sterile must be profound because a woman's worth is frequently measured by her fertility, and being sterile can be cause for a divorce.
It has been postulated that FGM may play a role in the transmission of HIV. One recent article which, was presented at the International Conference on AIDS 1998, was a study performed on 7350 young girls less than 16 years old in Dar es Salaam. In addition to other aspects of the research, it was revealed that 97% of the time, the same equipment could be used on 15-20 girls. The conclusion of the study was that the use of the same equipment facilitated HIV/AIDS/STD transmission.20
At the same conference, a research study performed in Nairobi indicated that FGM predisposes women to HIV infection in many ways (e.g., increased need for blood transfusions due to hemorrhage either when the procedure is performed, at childbirth, or a result of vaginal tearing during defibulation and intercourse, and the use of the same instruments for other initiates). Because FGM raises the social status of the parents, the dowry demands can be high and therefore the young girls can be married off to older men who are already infected.5 Contact with blood during intercourse is believed to be responsible for the transmission on HIV infection among homosexuals.21
Women who have had FGM done have a small opening, just large enough for the passage of urine and blood. Penetration or intercourse is difficult, often resulting in tissue damage, lesions, and postcoital bleeding. These tears would tend to make the squamous vaginal epithelium similar in permeability to the columnar mucosa of the rectum, thus facilitaing the possible transmission of HIV.22 The vaginal introitus is narrowed to increase the man's sexual enjoyment and ensure fidelity and virginity. However, because of the this many women experience severe dyspareunia.9,16 Other common reasons for the dyspareunia are epidermal or dermoid cysts, which form along the incisional site. These can be a small as a pea or as large as a football.13 These often become infected, painful, and a common reason for the woman seeking medical help. Dyspareunia can also be a result of neuromata that are formed when the dorsal nerve ending is trapped in scar tissue, resulting in immense pain and severe dyspareunia.23-25
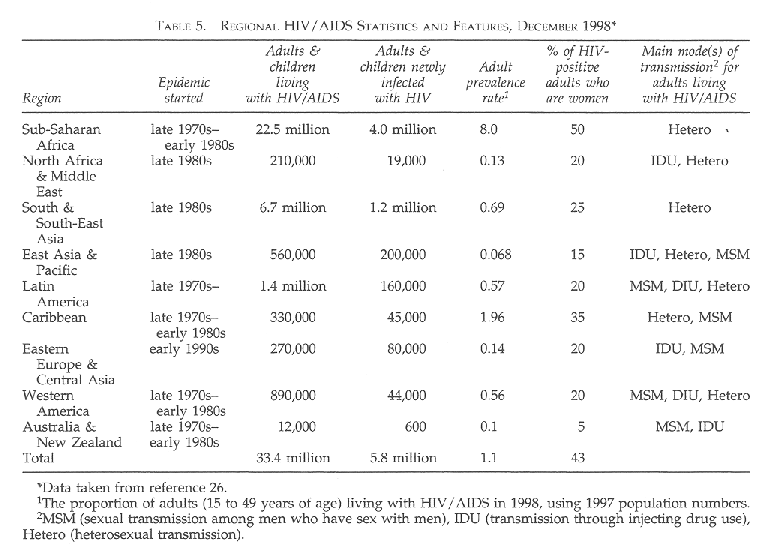
Unlike the rest of the world, sub-Saharan Africa has been more severely affected by HIV/AIDS. The sheer number of Africans infected is overwhelming. What is also of interest and concern is the number of women who are infected. The latest statistical data coming from WHO indicates that in Africa the ratio of male to female is 1:1, while in Europe and North America it is 4:1 (see Table 5). In Zimbabwe at 23 surveillance sites where the pregnant women were all tested anonymously for HIV, some 20-50% of them were found to be infected. At least one third of these women are likely to pass the infection on to their baby.26
Linke points to the common factor of contact with blood during intercourse for transmission of HIV in homosexuals in the United States and heterosexuals in Africa.21 For many of the women with FGM who have been infibulated (pharaonic), vagina intercourse is difficult at best and is associated with repeated tissue damage and bleeding, subsequently anal intercourse is resorted to with heterosexual partners. Thus the proposition that HIV transmission is enhanced because of the widespread practice of FGM.21,25
It is difficult for researchers to obtain accurate statistical data on anal intercourse for a host of reasons. Because of their cultural background, African women feel uncomfortable and shy discussing their sexual habits, and this is certainly true in the presence of males other than their husbands. Societal disapproval of anal intercourse is especially strong in areas where the majority of the population is Catholic, and admitting such behaviors can involve ostracization from the community.21 Moore et al.,27 in a study done on 1480 students in Zaire, found that 19% stated that they practiced anal intercourse. Because the question of homosexuality and anal sex is considered taboo, many Africans, male and female, are unwilling to discuss or admit to these practices, so these are believed to be grossly underreported. There is a large body of convincing evidence that genital ulceration and other STDs increase susceptibility to HIV infection.28 In reseach done by Allen et al.29 on HIV infection in urban Rwanda, the association between dyspareunia and nonmenstrual bleeding are often seen as signs and symptoms of undiagnosed venereal disease.29 In fact, in almost all of the research, genital lesions and ulcerations are discussed in the context of STD. The European study did report that in women with a history of candidiasis, the rate of HIV infection was significantly higher.30 As stated earlier and by many authors, included in the complications of HIV infection was significantly higher.30 As stated earlier and by many authors, included in the complications of FGM are severe dyspareunia, postcoital bleeding, ulceration and a high incidence of candidiasis.3,6,10,21,23,29 There is no conclusive evidence on the linkage of FGM to HIV transmission. However, Post31 describes an incident from a letter sent by the Minority Rights Group to Ammnesty International as follows: While in Malawi a couple of months ago, I came across the story of a 14 year-old girl of Yao tribe that inhabits land in the Southern end of the country. She was diagnosed as HIV-positive although she was a virgin. Blame was laid on the fact that during tribal circumcision, the same razor would be used on any number of children at the same time.
31 Perhaps future research on HIV transmission should include, as a variable, women who have had FGM performed because they also have genital ulcers and abrasions. If there were conclusive evidence linking FGM with the transmission of HIV, this may then become the best weapon in the arsenal for eradication of this practice.
There are many obstetrical complications associated with infibulation, for the mother and fetus/baby. However, Mawad and other authors11 stress that with careful planning, good antenatal, intrapartum and postpartum care, most of these can be avoided. Some of the main complications are delayed second-stage labor, perineal tearing, vesicovaginal fistula, and low birth weight babies. It has been reported that some pregnant women reduce their dietary intake to avoid giving birth to large babies.32 The obstetrical management for those patients is important and often difficult for those that have not had this type ofexposure.
The Norwich Park Hospital in the United Kingdom has established an African Well Woman Clinic
with a specially trained staff and protocols in place for the management of the FGM women. The necessity for this arose because of the high influx of immigrants from the Sudan and Somalia. These areas in Africa are where infibulation is practiced on at least 95% of the women. On staff there is a female Somali translator and a Sudanese psychologist. Since the clinic's inception the number of persons visiting the clinic has risen from under 1% to almost 6%. In the research done by McCaffery on 50 of the patients that attended the clinic, 13 were nonpregnant, 14 were primigravida, and 23 multigravida. The main reason for the nonpregnant women's attendance was to request defibulation. At first visit the average gestational age was 15-20 weeks. Of the 14 primigravida patients, 7 had an adequate introitus to facilitate first- and second-stage labor. One patient had a deinfibulation done earlier, two requested antenatal deinfibulation and three preferred the procedure to be done at the time of delivery (one patient did not return to the clinic). Thirteen (93%) primigravida patients had vaginal deliveries, and all of these had either episiootomies or perineal lacerations. Fourteen (61%) multiparous had vaginal deliveries. Six (25.1%) had caesarean sections, and with three (13%) instrumentation was used. Included in this research is an excellent in-depth discussion of the problems encountered and the obstetrical management Two cases are discussed in detail. The first was a 26-year-old Sudanese (primigravida) presented at 26 weeks gestation with severe vulval itching. The introital opening measured less than 1 cm, so a speculum exam was not possible. A swab was passed and cultured Candida albicans. However, the insertion of the applicator for clotrimazole cream was not possible. Because of the severity of her symptoms, the woman underwent defibulation at 28 weeks' gestation and subsequently had a normal vaginal delivery.
For the infibulated mother in labor with a narrow introitus, the inability to do a vaginal exam to monitor progress, apply fetal scalp electrodes, or blood sampling are for the obstetrician mid-wife serous reasons for concern. The second case discussed was that of a 20-year-old Somali primigravida admitted with contractions at full term. The introitus barely admitted one finger and cardiotocography of the fetal heart showed 60 bpm without a contraction. An epidural anesthesia was administered to facilitate vaginal exam, and at this time the cervix was 2 cm dilated. Artificial rupture of the membrane was performed and revealed thick black meconium. The decision was made to perform a cesarean section. However a catherization could not be done, so deinfibulation was carried out to facilitate this.33 The author while in Saudia Arabia in 1980, found that a urethral catherization on the infibulated woman was quite difficult and unsuccessful at times due to extensive scar tissue, bands, and anatomical distortion. Valuable time can be lost in an emergency. The staff at the African Well Woman Clinic have developed a high level of expertise in caring for the infibulated woman, and from research it is evident that they have incorporated all aspects of well-being including psychological and cultural. The staff strongly recommends antenatal defibulation or elective reversal either before pregnancy, at 20 weeks gestation or if seen later in pregnancy than at 38 weeks. It takes about 1 week for the reversal to heal. This procedure should be performed under spinal anesthesia because the sensation of touch triggers flashbacks of the infibulation in childhood. In the nonpregnant women, general anesthesia is recommended.
Many countries such as Canada, England, Sweden, Australia, and others have enacted statutes prohibiting FGM and reinfibulation after delivery. In the United States a law was passed in 1997 which criminalizes FGM performed on a person who has not reached the age of 18 years but it does not address women older than 18 or reinfibulation after delivery. Infibulation was made illegal in Sudan in 1946 and still today nearly 90% of the women in Sudan have been subjected to FGM.24 Because FGM is now illegal, many young girls are taken out of the country to have it performed. The Center for Disease Control and Prevention estimates that there are over 150,000 females at risk in the United States for undergoing FGM.35 Clearly it will take more than legislation to eradicate this practice that can no longer be seen as a religious or traditional custom. One cannot mount an ethical defense for a practice that results in such a negative impact on a woman's health. This is not only a problem for countries where it is performed, but also for the Western Countries.
Health-care providers have an important role to fulfill in the eradication of this practice. We should act as advocates and increase professional and public awareness about such a practice, explaining the dangers and life-long disabilities it imposes. Perhaps the well-known crusader for eradication of FGM, who herself had this done, Merserak (Mimi) Ramsey, spoke for all women when she said, This is a pain that doesn't go away. It is a lifetime wound,
36
KAPstudy. (Abst. Th C 105) Int Conf AIDS 1990;6:160.
Address reprint requests to:
Margaret Brady, Hostos Community College, 500 Grand Concourse, Bronx, NY 10451,
BradyFNP@aol.com
Comment in: AIDS Patient Care STDS 1999 Dec;13(12):683-8
The Circumcision Information and Resource Pages are a not-for-profit educational resource and library. IntactiWiki hosts this website but is not responsible for the content of this site. CIRP makes documents available without charge, for informational purposes only. The contents of this site are not intended to replace the professional medical or legal advice of a licensed practitioner.
© CIRP.org 1996-2026 | Filetree | Please visit our sponsor and host:
IntactiWiki.