American Journal of Diseases of the Child, Volume 134, Issue 7, Pages 676-678. July 1980.
American Journal of Diseases of the Child, Volume 134, Issue 7, Pages 676-678. July 1980.
* To assess the effect of pain on PaO₂ in newborns, transcutaneous PO₂ (tcPO₂) was monitored in ten healthy male infants undergoing circumcision. The tcPO₂ was seen to decrease to a lower level with pain and to remain low with continuing pain. After the circumcision, the tcPO₂ increased to levels equal to or exceeding those of the preoperative baseline period. Close concordance of tcPO₂ above and below the waist demonstrated no right-to-left shunting through the ductus arteriosus.
(Am J Dis Child 134:676-678, 1980)
Investigators1-5 who have correlated Pao₂ with transcutaneous Po₂ (tcPo₂) have obtained blood samples from indwelling arterial lines because of concern that the pain of an arterial puncture may disturb oxygenation. To further define the effect of pain on tcPo2, normal male infants were monitored during circumcision. Simultaneous monitoring of the tcPo2 over the right upper side of the chest and left lower part of the abdomen enabled us to evaluate the possibility of right-to-left shunting through the ductus arteriosus during the procedure of circumcision.
Ten healthy male infants were circumcised at 48 to 72 hours of age after obtaining informed consent from the parents. All were born at term with one-minute Apgar scores greater than 7 and a mean birth weight of 3,350 g. Neither heart murmurs nor abnormal femoral artery pulses were detected immediately prior to circumcision.
The procedure consisted of the following: about five minutes of cleaning the penis with povidone-iodine (Betadine) solution; adhesion lysis between glans and foreskin; dorsal foreskin clamping with forceps for two to four minutes followed by forceps removal and division of the crushed skin. A bloodless circumcision clamp (Gomco) was applied for five minutes before the foreskin was amputated. To discern the effect for each of the four painful manipulations, the interval from adhesion lysis to circumcision clamp removal was extended to 20 minutes.
Throughout the study, a radiant overhead warmer was used to maintain the abdominal skin temperature at 36.0°C. A nipple was offered for nonnutritive sucking. The period of continuous monitoring included at least 20 minutes before and after the circumcision. Transcutaneous oxygen electrodes (TCM1 Radiometer) were affixed below the right clavicle and to the left of the umbilicus. Both electrodes were thermally insulated with expanded rigid polystyrene plastic caps so that the electrode heat consumption served as an indirect measure of local blood flow.6 Respiratory and heart rates were monitored with vital signs modules. All parameters were recorded continuously on a potentiometric recorder. The tcPo₂ electrodes were interchanged at the end of the monitoring periods to help separate instrumentation from physiologic differences. Average values were obtained from planimetry of the tracings.7 Statistical comparisions used two-tailed τ testing.
Each of the studies demonstrated close concordance between the tcPo₂ tracings from the chest and abdomen (Fig 1). None of the infants showed a significant difference between chest and abdominal tcPo₂ during the quiet or crying intervals. Both tcPo₂ tracings decreased with pain and remained at a lower level until crying ceased. During brief respites from crying, the tcPo₂ was often exceeded.
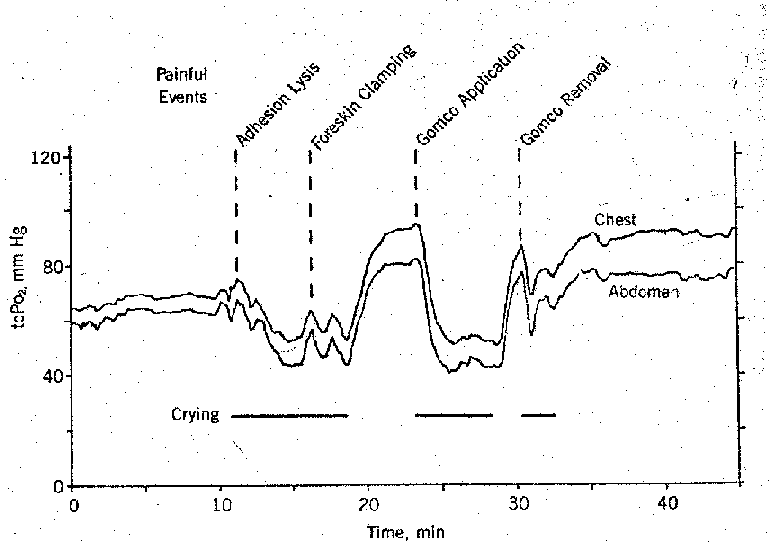
The change in tcPo₂ after the four painful procedures involved in circumcision was plotted for each of the ten subjects (Fig 2). There was a significant decrease in tcPo₂ for all 40 events considered together. (P<.001) and for three of the four individual categories. The average decrease in the tcPo2 was 15 mm Hg for adhesion lysis, less than 1 mm. for foreskin clamping, 13 mm Hg for circumcision clamp application, and 19 mm Hg for circumcision clamp removal. The negligible response to foreskin clamping probably reflects the absence of a quiet interval before this event in contrast to adhesion lysis and circumcision clamp removal, both of which followed manipulation-free intervals of five or more minutes, and circumcision clamp application, which was preceded by variable freedom from stimulation. The average postevent tcPo₂ for each of the four manipulations was not significantly different than that for any of the other three.
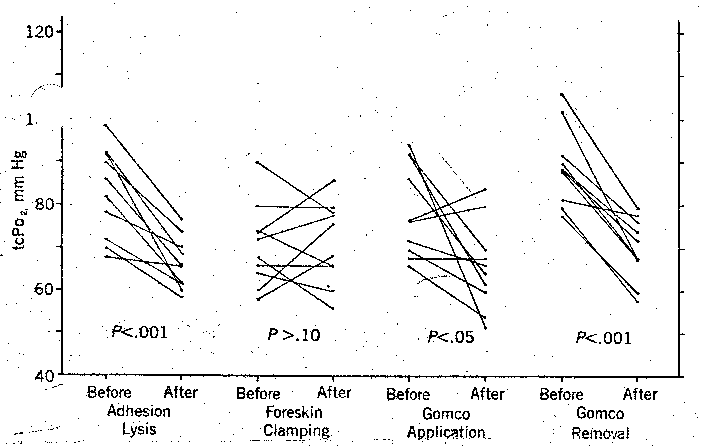
The average tcPo₂ was increased during the postoperative period. (P<.05, Table.).
Circumcision in neonates has been shown to affect adrenal cortical functions,8 immediate postoperative behavior and possibly long-term behavior.12 The present study demonstrates that circumcision also affects the heart rate, respiratory rate, and tcPo2 both during and immediately after the procedure. The observed decrease in tcPo2 with pain might result from momentary decreases in alveolar ventilation during crying. Right-to-left shunting at the atrial level, with crying, as shown by Lind et al.13 during the first two weeks of life, is also a possible explanation. The close concordance of chest and abdominal tcPo₂ indicates that despite vigorous crying right-to-left shunting through the ductus arteriosus did not occur in our sample of 2- to 3-day-old, term male infants. The absence of hypoxic symptoms in this group of term infants is in accord with our prediction that healthy infants should not be compromised by a transient decrease of 20 mm Hg in tcPo₂.
HEART RATE, Respiratory Rate and tcP₂ at Circumcision
Operative Periods
Before During After
Heart rate, beats/min
Mean 122 165* 138+
SD 26 21 28
Range 99-174 139-197 98-180
Repiratory rate, breaths/min
Mean 43 50+ 53+
SD 12 11 12
Range 22-64 39-77 40-79
tcPo₂
Mean 75 82 85+
SD 8 17 12
Range 62-88 66-129 65-106
*TcPo₂ indicates transcutaneous Po3, which was measured below right clavicle.
+Significantly (P<.05) greater than preoperative value.
The 10 mm Hg decrease in mean tcPo₂ after the circumcision could reflect increased minute ventilation in lungs fully expanded from recent crying. Although Martin et al.5 have also observed meant tcPo₂ less than 80 mm Hg in healthy infants, it is possible that an allowance should be made for the thicker skin of term infants since the electrode temperature of 44°C and the warm-up period of 20 minutes were based on correlation (r =.95) between the tcPo₂ and Pao₂ in premature infants.
The response to pain by each individual infant was surprisingly consistent. That is, some infants had abrupt decreases in tcPo₂ and increases in heart and respiratory rates with each of the painful stimuli while other infants repeatedly had attenuated responses. These individual variations in the response to pain underline the limited reliability of arterial punctures for assessment of resting Pao₂. Since the tcPo₂ often exceeded baseline values after crying ceased, there is also the possibility that delay in drawing an arterial blood sample could result in obtaining a Pao₂ that is greater than the baseline.
From the Department of Pediatrics, University of Michigan Medical School, Minneapolis, (Drs Rawlings and Engel); and
Hennepin County Medical Center, Minneapolis (Drs Rawlings, Engel, and Ms Miller).
Reprint requests to Hennepin County Medical Center, 701 Park Ave S, Minneapolis, MN 55415 (Dr Engel).
The Circumcision Information and Resource Pages are a not-for-profit educational resource and library. IntactiWiki hosts this website but is not responsible for the content of this site. CIRP makes documents available without charge, for informational purposes only. The contents of this site are not intended to replace the professional medical or legal advice of a licensed practitioner.
© CIRP.org 1996-2026 | Filetree | Please visit our sponsor and host:
IntactiWiki.