Journal of Family Practice, Volume 31, Issue 2, Pages 189-196. August 1990.
Seattle, Washington
Journal of Family Practice, Volume 31, Issue 2, Pages 189-196. August 1990.
Seattle, Washington
Information published in the last 5 years suggests a possible association between being uncircumcised and increased risk for urinary tract infection in the first year of life.1-4 Largely because of this data, the American Academy of Pediatrics convened a task force on circumcision, which released its findings in March of 1989. This group stated that circumcision may result in decreased incidence of urinary tract infection. However, in the absence of well designed prospective studies, conclusions regarding the relationship of urinary tract infection to circumcision are tentative.
They concluded: When circumcision is being considered, the benefits and risks should be explained to parents and informed consent obtained.
5
Alan Brett6 has recently written an editorial entitled How Should Practicing Physicians Interpret the Published Data for Patients?
Although his subject matter is different from that of this paper, in addressing the question his title poses, Brett offers the reader some observations and approaches that are highly useful here: Intervention based on risk factors differs qualitatively from treatment of an already manifest disease. It offers specific people therapeutic manipulations on the basis of statistical risk, not existing illness. ... As long as a recommended type of behavior is at worst harmless, it may be ethically imposed without unequivocal proof of benefit; the possiblity of benefit may suffice.
He notes that a strongly interventionist perspective may color the published findings of large trials, and he suggests three perspectives from which to interpret data to patients: (1) the relative differences between cases and controls, (2) the absolute differences between cases and controls, and (3) those without the morbid event and htose who, having had the intervention, still experience the morbid event.
This general approach is used in the review that follows, in which the prepuce (foreskin) as a risk factor for urinary tract infection in male children for the first year of life is considered.
The available data are summarized in Table 1. Ginsberg and McCracken7 in 1982 described a case series of infants 5 days to 8 months of age hospitalized with urinary tract infections. Sixty-two of these subjects were male and only three were circumcised. This finding led the authors to conclude that it is tempting to speculate that the uncircumcised male has an increased susceptibility to UTI.
Subsequently there has been a series of three papers published by Wiswell and colleagues1-3 from Brooke Army Hospital and various other army hospitals using retrospective cohort methods for children hospitalized with urinary tract infection in the first year of life. Only crude analyses are persented for the comparison of urinary tract infections in circumcised and vs uncircumcised infants. No attempt was made to control for age, race, education, or income in these analyses. When this omission was pointed out to the authors, they replied that what we found in our study population was that the circumcision frequency rate did not significantly vary between socioeconomic groups.
No data have been produced however, to document this assertion.8
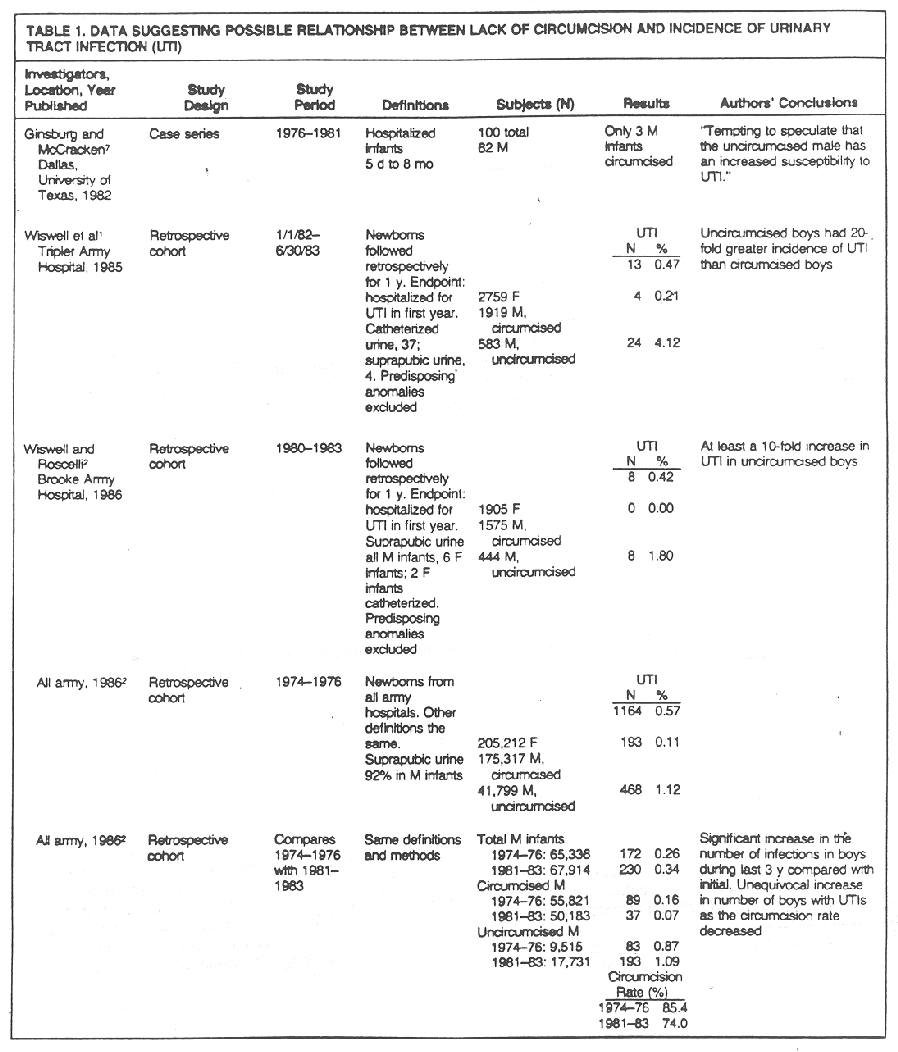
To be convincing, the authors would need to present the data with an adjustment for those socioeconomic factors of significance, especially in view of the report from the National Health Examination Survey of 6768 boys 12 to 17 years old who were examined during the 1966-1970 examination cycle. Circumcision rates were 75% overall, but there were absolute differences ranging between 30% to 60% by income and education and between blacks and whites.9 The role of these factors could be important, since other heath-seeking behaviors are quite likely to vary with them. For example, uncircumcised children from families with lower income and educational levels might well be brought for medical care at a later time in the progression of their illness, resulting in disproportionate hospitalization rates. It is known that not all children with urinary tract infections are hospitalized; in Herzog's study from Boston Children's Hospital,4 19% were not. In addition, the work of Wiswell and colleagues does not take into account the possibility of differences in the health-care-providing behavior of physicians (eg, the use and timing of bag or suprapubic urine collection for diagnosis), which could result in different hospitalization rates between circumcised and uncircumcised male infants. Only population-based or prospective studies conducted in a manner similar to the study of Wettergren and others10 can address or avoid this potential source of bias.
The interventionist sentiment mentioned by Brett is apparent in the writings of the Wiswell groups. In the 1986 paper Wiswell and Roscelli2 reported that there was an unequivocal increase in the number of male urinary tract infections as the circumcision rates decreased.
The actual rate changed from 0.26% to 0.34% in all male infants, comparing the 1974 to 1976 period with the 1981 to 1983 period. The P value for this change based on chi-square is .02. It is well known, however, that if large enough numbers are used, statistical significance may be achieved when biological significance is lacking. A more instructive way to examine the change is achieved by calculating the relative risk for urinary tract infection over the two periods. The relative risk then becomes 1.28 for the increase with a 95% confidence interval of 1.09 to 1.52. The lower boundary of this confidence interval suggests that the effect, if unbiased, is small. While emphasizing the change in total urinary tract infection rates over time, the authors failed to mention a much larger apparent change in the rate of urinary tract infection from time 1 to time 2 in circumcised infants (from 0.16% to 0.07%). The resultant relative risk for urinary tract infection in circumcised infants in the second period is 0.46 with a 95% confidence interval of 0.33 to 0.63. Since urinary tract infection is a biological event in either circumcised or uncircumcised boys, the rate in either of those subgroups should be relatively constant over time. When this finding was brought to the author's attention, they suggested that a 0.21% rate for uninary tract infections in circumcised boys was aberrant and led to the erroneous impression
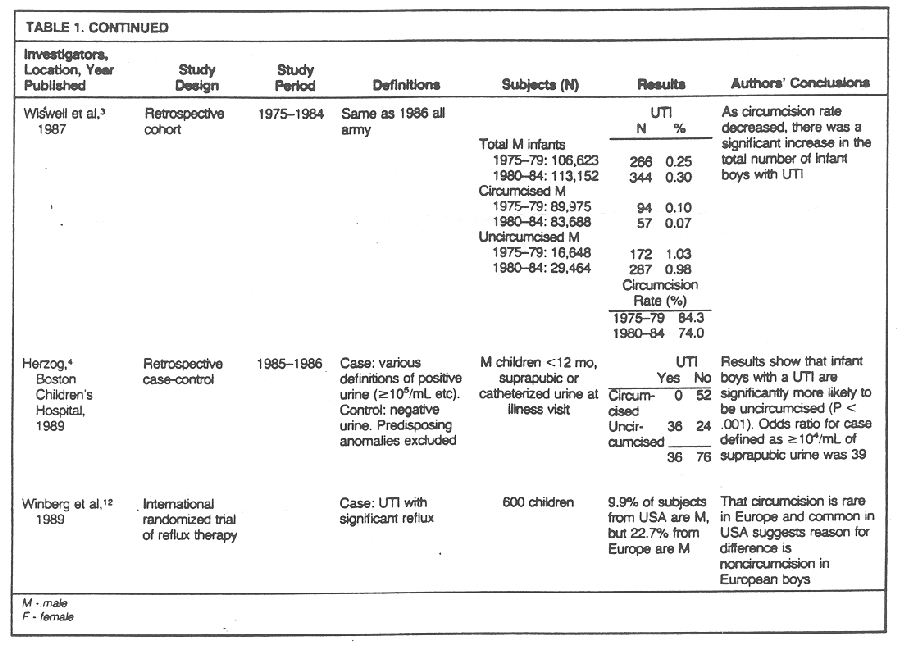
of change mentioned above.8 In further analyses from this group the year 1874 has been dropped (see the 1987 publication).3 Clearly by leaving out the 1974 year, the graphic representation of the data looks better. In further correspondence Wiswell11 desccribes the US army hospitals' experience from 1971 to 1986. He reports that the rate of urinary tract infection in their series of circumcised boys has ranged from 0.07% to 0.13%. The rates are said to be relatively constant.
3 The rates are not constant. Two- to threefold differences in year-to-year rates derived from these large data sets imply problems with the data.
Herzog,4 from Boston's Children's Hospital, in 1989 reports a retrospective case-control study in which cases were found by examining the results of all suprapubic and catherized urine specimens obtained in the emergency department as part of illness workup in male children up to 1 year of age. Case patients were defined as those with greater than 100,000 organisms per milliliter. Control patients were individuals with negative urine samples. An attempt was made to control for the effects of ace, race, and medical insurance source as a proxy for income. For 36 cases, in which none of the infants were circumcised, and 76 controls, the differences in the circumcision rates between cases and controls were highly significant (P<.001). It was reported that there was no significant differences to be found in the two groups in age, ethnic group, and type of medical insurance.
In 47% of the cases, however, the infants were less than 3 months of age, while only 39% of the control patients were that young; 47% of the case patients were Hispanic, 28% were black, and 19% white, whereas the respective percentages for the control patients were 17%, 34%, and 47%; 50% of case patients were on Medicaid insurance compared with 33% of the control group. The overall numbers of subjects in this study are small, so none of the above differences was statistically significant; however, the odds ratio for non-white vs white ethnic differences between case patients and control patients was 3.0 (95% confidence interval 1.2 to 7.1), which suggests a true difference. One would be more confident of the results of the statistical analysis had been adjusted for age, ethnicity, and type of medical insurance. Another potential source of bias in this study was the loss of nearly one quarter (23%) of the potential control subjects for whom circumcision status could not be determined. Finally, the general comments about potential biases attributable to health-care-seeking and health-care-providing behaviors raised earlier are applicable to this study as well.
The final piece of evidence presented in Table 1 is reported by Winberg et al12 from the randomized treal of reflux therapy. Of the 600 children entered into the trial so far with urinary tract infection, 9,9% of the subjects from the United States are male, where most male infants are circumcised, and 22.7% from Europe are male, where most infants are not circumcised. These results of suggestive of the association between lack of circumcision and urinary tract infection.
Another line of evidence comes from comparison of symptomatic urinary tract infection rates in different geographical areas of the world. The incidence of symptomatic urinary tract infections in Swedish infant boys is 1.2%10 (nearly all uncircumcised), a rate comparable to that reported overall by Wiswell11 of 1.15% for uncircumcised boys. Similar rates have been reported from Austria and Germany.11,13
Work in recent years on the pathogenesis of urinary tract infections from a number of national and international sources lends plausibility to a possible association between lack of circumcision and urinary tract infection. The evidence suggests that infection is the result of gastrointestininal population from the environment by pathogenic organisms (most notably pyelonephritogenic, P-fimbriated Escherichia coli) with subsequent colonization of the periurethral area followed by ascending infection. Pyelonephriticgenic E. coli have been shown to colonize the periurethral and fecal flora in nearly 100% of cases of acute febrile pyelonephritis as compared with 10% in healthy controls.12,14-19 Indeed, if the gut-colonizing bacteria of the newborn are P-fimbriated E coli strains, nosoconomial outbreaks of pyelonephritiscan occur.20
The various lines of evidence reviewed above have caused Winberg and coworkers12 to post the question, Is the prepuce a mistake of nature?
They argue that a mistake is improbable, and propose as the explanation that one unphysiological intervention (circumcision) is counterbalancing the effect of another, namely the exposure to the microbial environment of the modern maternity unit. They base their hypothesesis on four observations. First, in biological settings, when the mother gives birth in the squatting or kneeling position, she rapidly transfers her largely anaerobic and non-E coli gut flora to the child during the process of delivery. Second, the child's gastrointestinal tract is the probable source of bacteria, and the male prepuce becomes heavily colonized with E coli during the first few days of life. Third, this colonization arises because E coli and P-fimbriated strains, in particular, bind avidly to the prepuce. Fourth, infantile pyelonephritis is due to a P-fimbriated E coli strain in about 90% to 97% of cases. Winberg and colleagues suggest two alternative approaches to the problem of urinary tract infections in infants aside from possible protection through circumcision: (1) an experimental approach of attempting to populate the newborn gut with less pathogenic bacteria while in the nursery, and (2) a practical approach of providing strict rooming-in to increase the likelihood of the baby being colonized by material strains as suggested by the work of Bettleheim and coworkers.21
In summary, then, the various lines of evidence, ranging from case series reports to retrospective cohort and case-control studies to international geographical comparisons and studies of pathogenesis, suggest an association between uncircumcised status and increased incidence of urinary tract infection. It is clear from the above review that these data do not constitute the unequivocal proof
required by Brett before proceeding with an intervention that is not harmless (circumcision) directed to the risk of urinary tract infection in the first year of life.
Simonsen and coworkers,22 in attempting to explain the different pattern for AIDS transmission in Africa as compared with that of the United States, performed a case-control study on 340 men reporting to a sexually transmitted disease clinic in Nairobi, Kenya. These men had very low rates for homosexuality and intravenous drug use. In an analysis controlling for potential differences in age, marital status, years living in Nairobi, travel outside of Kenya, age at first intercourse, number of lifetime sexual partners, frequency of contact with prostitutes, and lack of circumcision, the relative risk for human immunodeficiency virus was 2.7 for uncircumcised men.22 According to a research news article in Science (August 1989),23 similar studies tend to confirm these findings in Africa. The results in the United States are conflicting.
The possible benefits of an intervention (circumcision) have been considered. Now to address the price that some individuals pay if this intervention is undertaken. One universal complication of circumcision is pain.24,25 Dixon and others26 performed blinded Brazelton assessments on babies repeatedly before and after circumcision and uncircumcision and reported that circumcision results in disruptions in the children's behaviorand recovery reactions for 24 hours or more.
In Table 2 the common and more serious early and late complications of circumcision are portrayed. The complications have been grouped into three categories: hemorrhage, infection and surgical trauma. Surgical trauma includes removal of too much or too little skin, injury to the urethra or glans, would dehiscence, circumcision of a child with hypospadias, and the like. The data are based mainly on recent reports on circumcisions performed in the neonatal period. Gee and Ansell27 reported the experience at the University of Washington nurseries for 5521 newborns circumcised at that institution from 1963 to 1972. The total rate of complications in this series was 1.9%. Fourteen of the complications in this series (0.2%) were gravely serious: 1 life-threatening hemorrhage, 4 systemic infections, 8 circumcisions of infants with hypospadias, and one complete denudation of the penile shaft. Metcalf et al,28 at the University of Utah, using interviews, questionaires, and chart reviews on an outpatient population, got a total rate for hemorrhage, infection and trauma of about 4%. Harkavy29 reported on 4000 circumcisions with an incidence of 0.6 percent for notifiable complications, mostly bleeding.
It is not totally clear from his report what notifiable
means, but the impression is that the physician had been notified about the particular complication. Wiswell and Geschke30 reported on over 100,000 newborns from all army hospitals for the years 1980 through 1985. they sought only complications specifically recorded as such in the first month of life. Their total rate for the three groups of complications is about 0.19%, probably reflecting the stringency of he criteria and recording practices of the physicians involved. Late complications tend to divide themselves into three groups: the need for surgical revision; the presence of adhesions, skin bridges, and the like; and the occurence of meatitis. Later surgical revision, usually requiring general anesthesia is required approximately 1% of the time,28,31 as was shown in two studies, one in the United States,28 with a sample size of 230 outpatients, the other in England, with a random population-based sample of 2428 boys.
Investigator Year Sample Size and Surgical Total
Published Nature of Study Hemorrhage (%) Infection (%) Trauma (%) Rate (%)
Gee and Ansell,27 1978 5521 newborn boys 1.07 0.42 0.40 1.9
University of Washington Record review,
complications sought
out in whole record
Metcalf et al,28 1983 361 including 2.0 1.0 1.0 4.0
University of Utah interviewed
outpatients
Harkavy,29 1987 4000 newborns "notifiable complications mostly bleeding"
Georgetown University
Wiswell and Geschete30 1989 100,157. All army, 0.06 0.07 0.025 0.19
1980-1985. Boys <1
mo. old. Only if
recorded as a
complication
*Surgical trauma in this context includes removal of too much or too little skin, injury to the urethra or glans penis, circumcision in child with hypospadias, wound dishiscence, pneunothorax.
The articles cited in Table 2 give a general sense of what one may expect in the way of common and moderately severe early complications of circumcision. Extensive reviews25,32,33 list many more potential complications, but these seem to be quite rare. Death as a complication from newborn circumcision has been estimated to occur in from 1 in 24,000 to 1 in approximately 500,000.30,33 Some investigators have actively sought out complications by interview and have recorded rates of 55%.34
In Table 3 the above question is approached by considering a hypothetical cohort of 2000 newborn male infants, 1000 of whom are circumcised and 1000 of whom are not circumcised. If one accepts the suggestive evidence presented by Wiswell and others as reviewed earlier, one can estimate that the relative differences for these two subcohorts will be a possible 10-fold relative increase in urinary tract infections in the uncircumcised male infants in the first year of life.1-4 From the prospective of absolute differences, there will be 9 more urinary tract infections per 1000 newborns not circumcised. From the perspective of those without the morbid event (UTI), these data mean that 99.9% of circumcised infants will not experience the morbid event, while for the uncircumcised the figure would be 99.0%. As noted in Table 3, the absolute benefit (possibly 9 infants will have urinary tract infection prevented) is weighed against the price paid by those experiencing the intervention (990 individuals circumcised who do not get urinary tract infections plus 1 who was circumcised and experiences a urinary tract infection in the first year of life) without any benefit to them. The price paid by the 991 receiving no benefit depends on the rates of complication. Three possible rates for early (0.2% from Wiswell and Geschke,30 2% from Gee and Ansell,27 4% from Metcalf et al28) and 1% for late complications have been examined.28,31 At the lowest rate for early complications (0.2) three more individuals on balance will have moderately severe to very severe complications from circumcision than will benefit from circumcision. At the other extreme (4% early complications), the result will be 41 more individuals moderately or severely adversely affected bycircumcision than the 9 who may benefit.
Table 3. EXAMINATION OF POSSIBLE ASSOCIATION BETWEEN URINARY TRACT INFECTION (UTI) AND NONCIRCUMCISION IN A HYPOTHETICAL COHORT OF 2000 NEWBORN IN THE FIRST YEAR OF LIFE, WITH 1000 CIRCUMCISED, 1000 UNCIRCUMCISED.
Relative Differences UTI Rate Comment
Circumcised 0.1 Possible 10 fold
Uncircumcised 1.0 relative increase in
uncircumcised boys.
Absolute Differences UTI (No/%) Possible absolute
difference of
Circumcised 1 0.1 0.9% (9/1000) between
Noncircumcised 10 1.0 circumcised and
uncircumcised boys.
Perspective of Those Nonevent Possible boost in
without the morbid Probability chances of no
Event UTI in first year from
99% to 99.9%
Event (no UTI)
Circumcised 999/1000
Noncircumcised 990/1000
Weighing absolute benefit against absolute price paid by
those experiencing the intervention without benefit to them
for a cohort of 1000 circumcised male infants.
Possible absolute benefit 9 UTIs possibly
averted
Price in circumcision
complications for 991
with no benefit
If incidence is:
0.2 2% 4%
Early: hemorrhage,
infection,
surgical trauma Number 2 20 40
Late: surgical 1%
revision Number 10 10 10
Balance of benefits -3 -21 -41
to complications.
(Number of
individuals)
Complications: hemorrhage, infection, or surgical trauma
(See footnote Table 2 for definition of surgical trauma.)
It can be argued that the gravity of urinary tract infections in infancy (<1 year of age), and the neonatal period(<30 days) in particular, is so significant as to outweigh numerical comparisons such as those in Table 3. Two questions seem relevant. How common are neonatal urinary tract infections in uncircumcised male infants? From the work of Bergstrom and colleagues,35 Wiswell and Geschke,30 and Ring and Zobel,36 the incidence can be estimated at from 1.6 to 2.4/1000. This range is comparable to the yearly incidence rate of breast cancer or colon cancer in middle aged adults and is more common than neonatal hypothyroidism. The second question is, how serious is a neonatal urinary tract infection? The answer to this question is less clear. From the data of Wiswell and Geschke,30 the population-based mortality rate for uncircumcised male infants is 5.5 in 100,000 or about 1 in 18,000. The case fatality rate for their series was 1.9% (2/108). Other recent population based data was not found in the literature. Case fatality rates for case series are available, however. In the pre-antibiotic era Craig37 reported a case fatality rate of 15%; Littlewood38 reported a case fatality rate of 7.6% in a series from 1950 to 1968. Davies and Gothefors,39 in their review of newborn infections, concluded that the immediate prognosis should be uniformly favorable except in children with serious malformations or other underlying conditions. In summary, neonatal urinary tract infection is not a common event; the prognosis in the modern era is potentially serious, but not easily quantifiable.
Unequivocal proof that lack of circumcision is a risk factor for increased urinary tract infection is currently unavailable. Intervention based on risk factors differs qualitatively from the treatment of already manifest disease.
6 The standard to be met is higher; it has not been met. The behavior change suggested (circumcision) is not harmless and therefore cannot be recommended without unequivocal proof of benefit. The rate of non-event (no urinary tract infection) may be increased from 99.0% to 99.9% by circumcision. The price of a potential benefit to 9 in 1000 will be numerically overbalanced by the moderately severe to severe complications (early and late) even if the rate for early complication is as low as 0.2%
Specific information to be offered to parents should include the following:
Nature is a possessive mistress and whatever mistakes she makes about the structure of the less essential organs such as the brain and the stomach, and in which she is not much interested, you can be sure that she knows best about the genital organs,40
Submitted November 17, 1989.
From the Department of Preventive Care, Group Health Cooperative of Puget Sound, Seattle, Washington. Requests for reprints should be addressed to Robert S. Thompson, MD, Department of Preventive Care, Group Health Cooperative of Puget Sound, Suite 1600, Metropolitan Park II, 1730 Minor Ave, Seattle, WA 98101-1448.
The Circumcision Information and Resource Pages are a not-for-profit educational resource and library. IntactiWiki hosts this website but is not responsible for the content of this site. CIRP makes documents available without charge, for informational purposes only. The contents of this site are not intended to replace the professional medical or legal advice of a licensed practitioner.
© CIRP.org 1996-2026 | Filetree | Please visit our sponsor and host:
IntactiWiki.