ANZ Journal of Surgery, Volume 73, Issue 8: Pages 610-614, August 2003.
ORIGINAL ARTICLE
KATRINA SPILSBURY, *JAMES B. SEMMENS, *Z. STAN WISNIEWSKI and C. D'ARCY J. HOLMAN*
*Western Australian Safety and Quality of Surgical Care Project, Centre for Health Services Research, School of Population Health, University of Western Australia, Crawley and Western Australian Safety and Quality of Surgical Care Committee, Royal Australasian College of Surgeons, Western Australian Branch, Nedlands, Western Australia, Australia
Background: Routine neonatal circumcision has declined in most English-speaking countries. The purpose of the present study was to investigate the trends in incidence of routine circumcision in Western Australia and current patterns of the procedure according to sociodemographic factors.
Methods: Hospital morbidity data were used to conduct a population-based study of all circumcisions performed in Western Australian hospitals during 1981-1999. Medicare insurance rebate statistics were used to estimate the numbers of circumcisions performed outside of hospital on boys <6 months of age between 1994 and 1999.
Results: In 1994, 9.8% of boys were circumcised before reaching 6 months of age, falling to 7.9% by 1999. Boys <6 months of age were 3.3 times more likely to undergo a hospital-performed circumcision if they lived in country areas compared with metropolitan Perth. Middle socioeconomic class families were twice as likely to circumcise a son than those in the higher and lower socio-economic groups. The decreasing circumcision rate in boys <6 months of age was partly offset by an increase in routine circumcisions in boys older than 6 months of age during 1981-1999.
Conclusion: Circumcision remains a relatively common procedure in Western Australia. Based on total routine circumcision rates in 1999, 10.2% of boys will be circumcised by the time they reach 15 years of age. The routine circumcision rate in boys <6 months is falling in contrast to a rising routine circumcision rate in older boys. Risk factors for a circumcision before 6 months of age include living in country areas and a middle socioeconomic status.
Key words: epidemiology, linked data, routine circumcision, Western Australia.
Abbreviations: CI, confidence interval; GP, general practitioner; ICD, International Classification of Diseases; RR, rate ratio.
Circumcision of boys is widely practised throughout the world, with an estimated one-sixth of the world's men having undergone the procedure.1 The practice of circumcision dates back many thousands of years and has been carried out for ritual, religious, cultural and medical reasons. Today, religious beliefs prescribe circumcision of Jewish and Muslim boys and some tribal cultures perform circumcision as a rite of passage in early adult life.2,3 Circumcision first became a routine medical procedure in English-speaking countries in the late 19th century, supposedly to prevent masturbation and cure conditions such as alcoholism and rheumatism.4 The practice further proliferated during the World Wars I and II with the view that it could improve hygiene and prevent venereal disease. The result of its widespread practice was the acceptance of circumcision as a social norm for the majority of newborn boys in most English-speaking countries. A controversial study by Gairdner in 1949 questioned neonatal circumcision, a practice that had led to the death of 19 English boys under age 5 years in 1946.5 Neonatal circumcision has since declined in England, to <1% by 1985.4 Similarly, in New Zealand the practice of neonatal circumcision has fallen sharply. In 1979, one study reported that 25% of infants were circumcised, while 62% of their fathers had been circumcised.6 Based on hospital morbidity (New Zealand Health Information Service, unpubl. data, 2001)7 and population data,8 in 1995 <0.5% of boys <5 years of age were circumcised in New Zealand hospitals. Circumcision remains more prevalent in Canada and the USA although declining rates have been reported. The proportion of newborns circumcised in Ontario, Canada, fell from 53% in 19799 to 44% in 1994,10 while in the USA it was estimated that approximately 80% of newborns were circumcised in 19804 compared with 61% in 1992.11 Australia has also reported a decline in neonatal circumcision, from 50% to 24% during the period 1974-1983.12 No recent estimates of neonatal circumcision have been reported from Australia.
In agreement with medical associations in Canada,13 England 14 and the USA,15 the Australasian Association of Paediatric Surgeons states that neonatal circumcision has no medical indication and does not support the routine circumcision of newborn boys in Australia. It also recommends that elective circumcisions be carried out after 6 months of age.16 These recommendations are based on evidence that weighs the advantage of potential health benefits against the disadvantage of potential health complications, health-care costs and the legal issues of performing an unnecessary procedure on a minor. Given this lack of endorsement and the falling trends observed in other countries, it was expected that the rate of routine circumcision in Western Australia would have fallen since the last published statistics of 1983 and that the rate is continuing to decline.
As part of the Western Australian Safety and Quality of Surgical Care Project17 the objective of the present study was to conduct a population-based review of the current incidence rates, trends and factors associated with the circumcision of boys <6 months of age and boys 6 months and older, but <15 years in Western Australia between 1981 and 1999. The Western Australian Health Services Research Data Linkage System (WA Data Linkage System) was used to access hospital separation data based on a population of 1.9 million people spanning a 19 year period.18
The WA Data Linkage System was used to extract hospital morbidity data on all boys circumcised in 1981-1999. Morbidity records were selected using the International Classification of Diseases (ICD) procedure codes for circumcision (ICPM 5-640,19 ICD-9-CM 64.020 or ICD-10-CM 30653-0021). Circumcisions performed during the birth admission were not recorded in the WA Data Linkage System prior to 1992, which restricted analysis of boys <6 months of age to 1993-1999. Medicare rebate data from the Health Insurance Commission (Canberra, Australian Capital Territory) was used to estimate the number of circumcisions performed out of hospital (private rooms and general practitioner (GP) surgeries) on boys <6 months old. The total number of circumcisions on boys <6 months old was estimated by summing the number of publicly insured hospital patients and the number of Medicare claims from 1994 to 1999. All analysis was performed on anonymous data current to 31 December 1999.
Statistical analysis was performed using SPSS22 and incidence rates over the 19 year study period calculated using the RATES CALCULATOR program.23 Hospital location was used to assign a metropolitan or country hospital identifier. Patient postcodes were used to assign one of eight health service zones: the Perth metropolitan area and seven country areas (two remote regions, Kimberley and Pilbara, and five rural regions: Midwest, Central, South-west, Great Southern and Goldfields). A Socio-Economic Index of Disadvantage level derived from characteristics such as income, educational attainment, unemployment, and occupation, as determined by the Australian Bureau of Statistics from the 1996 census,was also assigned using patient postcodes. The numbers of male births grouped by year and postcode were obtained from the Health Department of Western Australia and were used as the denominators in the socioeconomic analysis. Logistic regression was used to estimate the relative risk of circumcised boys 6 months and older but <15 years being Aboriginal and/or Torres Strait Islander. Admissions with more than one ICD procedure code and circumcisions during the birth admission were excluded from length of stay analysis. Day surgery procedures were counted as 1 day hospital stays.
The total number and length of stay in hospital were estimated using both routine and medically indicated circumcisions. All age-specific trends were confined to routine circumcisions only. A routine circumcision in the present study was defined as any circumcision with an ICD diagnosis code for a routine circumcision (ICD-9 V50.2, ICD-9-CM V50.2 or ICD-10-CM Z41.2) or any circumcision performed in the absence of a medically indicated diagnosis code for penile disorders including phimosis, balanoposthitis, balanitis xerotica obliterans, hypospadias, other congenital disorders, vascular disorders, atrophy, fibrosis, ulcer, hypertrophy, priapism, abscess, boil, carbuncle, cellulitis, penile cancer or other unspecified penile disorders. Trends in the rate of circumcision for medically indicated reasons in Western Australia have been published elsewhere.24
There were 25 718 index admissions recorded for circumcision in Western Australian hospitals in 1981-1999. After using Medicare rebate data to include those additional procedures performed outside of the hospital system, it was estimated that an average of 2370 (SD ± 62) circumcisions was performed annually during 1994-1999 with 1490 (SD ± 71) of those performed for routine reasons. Seventy-six per cent (1132 ± 80) of routine circumcisions were performed on boys <6 months of age. The average length of stay in hospital for a circumcision fell from 2.7 days in 1981 to 1.0 days in 1999 (mean difference, 1.7 days; 95% confidence interval (CI):1.3-2.1). The cumulative risk of routine circumcision, based on 1999 data, was 10.2% by 15 years of age.

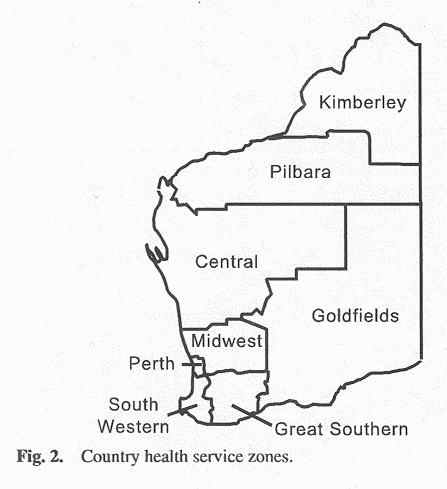
For boys <6 months of age, the routine circumcision rate decreased by a geometric average of 3.8% per calendar year (95%CI: 2.4-5.1%) from 9.8 per 100 person-years in 1994 to 7.9 per 100 person-years in 1999 (Fig.1). The decline was more marked for hospital-performed circumcisions, which fell by 8.1% per year (95%CI:5.5-10.6%). Of the 4109 circumcisions performed on boys <6 months between 1993 and 1999 in Western Australian hospitals, only 20 Aboriginal and/or Torres Strait Islander boys (0.5%) were identified. The number of circumcisions performed outside of a hospital remained stable over the time period (95%CI: -1.5-2.6%).
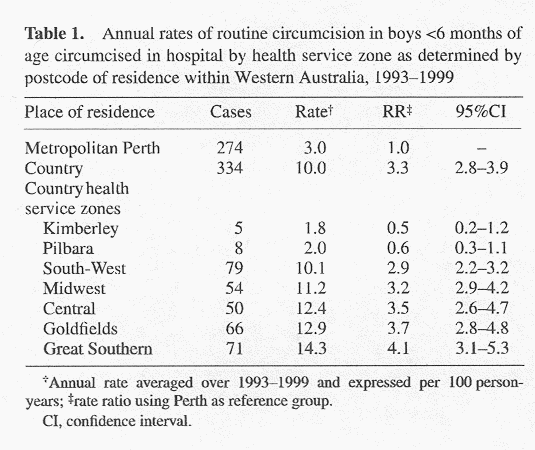
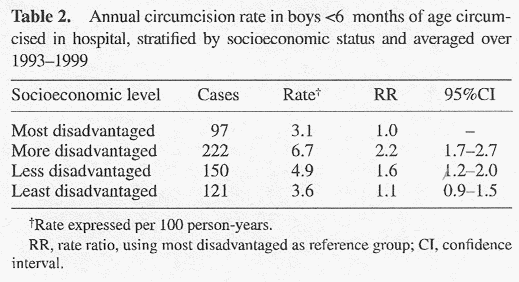
In general, boys <6 months of age living in country areas of Western Australia were 3.3 (95%CI: 2.8-3.9) times more likely to have an in-hospital circumcision than boys in the Perth metropolitan area in 1993-1999 (Fig.2; Table 1). Further breakdown of country Western Australia into seven health service zones showed a wide variation in routine circumcision rates between populations resident in different regions. The two northern and most remote health service zones, the Kimberley and Pilbara, had routine circumcision rates similar to the Perth metropolitan area. The other five more rural health service zones had hospital rates of routine circumcisions three to four times higher than in the Perth metropolitan area.
The annual circumcision rate in boys <6 months of age was also calculated by socioeconomic level and compared with the circumcision rate in the most disadvantaged (Table 2). The two middle socioeconomic levels had higher rates of circumcision compared with the lowest socioeconomic ranking (rate ratio (RR)=2.2, 95%CI: 1.7-2.7; RR = 1.6, 95%CI: 1.2-2.0). There was no difference between the most and least disadvantaged groups (RR = 1.1, 95%CI: 0.9-1.5).
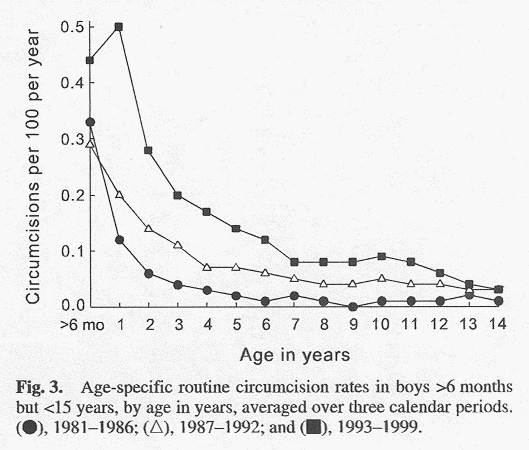
As boys grew older than 6 months, the rate of routine circumcision decreased exponentially (Fig.3). In 1993-1999 the rate of routine circumcision of 1-year-old boys was 0.5 per 100 person- years, declining to 0.03 per 100 person-years by age 14 years compared with 9.3 per 100 person-years in boys <6 months of age. This declining trend by age was observed also in the earlier calendar periods 1981-1986 and 1987-1992. In contrast, the rate of routine circumcision increased with calendar period in boys at any individual age. The largest increase was observed in 6-year-old boys with 0.01 circumcisions per 100 person-years in 1981-1986,increasing 12-fold (95%CI: 5.6-4.6) to 0.12 per 100 person-years by 1993-1999.
Based on hospital records, 15.8% of all routine circumcisions on boys 6 months and older but <15 years were performed on Aboriginal and/or Torres Strait Islander boys. Most of these boys (96.6%) were living in rural Western Australia at the time. The relative risk of boys older than 6 months but <15 years being Aboriginal and/or Torres Strait Islander when circumcised decreased by 27% (95%CI: 4.2-56.7) with each more recent calendar period, indicating that the increased circumcision rates in older boys was a result of more non-Aboriginal boys being circumcised. A boy circumcised when aged 10-14 years was 23.7 (95% CI:16.8-33.5) times more likely to be Aboriginal and/or Torres Strait Islander compared to a boy circumcised between 6 months and 4 years of age, after adjusting for calendar period and location.
There was a 20% decline in the rate of circumcision of Western Australian boys <6 months of age from 1994 to 1999 with approximately 8% currently being circumcised. This trend continues the 50% decline reported in neonatal circumcisions from 1974 to 1983.12 The rate of circumcisions performed in hospitals fell faster than those performed out of the hospital system.
A marked dichotomy exists between the rates at which boys <6 months of age from country areas were circumcised compared with those from the Perth metropolitan area. Approximately 72% of the Western Australian population reside in metropolitan Perth. In 1993-1999, a boy <6 months of age and living outside of Perth was more than three times as likely to be circumcised in hospital than a metropolitan boy of the same age.
There are several possible explanations for the difference in circumcision practice between country and metropolitan Western Australia. First, GPs in country Western Australia are more likely to be older and male,25 and thus are more likely to be circumcised than Perth doctors and perhaps be more willing to perform the procedure. Second, multicultural variation between the metropolitan and country populations may explain some differences in circumcision practice. This hypothesis is supported by census data showing that 36% of Perth residents were born overseas, mostly from European countries that do not practice routine circumcision. Residents of country regions were more likely to have been born in Australia, with 21% born elsewhere. Last, it may be easier for parents in Perth to access physicians who are willing to perform circumcisions outside of the hospital system compared to country areas, which would reduce the rate of circumcisions performed in Perth hospitals compared with country hospitals. A more detailed study would be needed to confirm this.
Variation in the rate of circumcision of boys <6 months of age was observed between different country regions of Western Australia. The remote northern regions had rates of routine circumcision comparable to metropolitan Perth, while circumcision was significantly more common in the central and southern rural areas. The lower rates in the north were most likely due to the different population distribution. Approximately 35% of the population living in the Kimberley are Aboriginal and/or Torres Strait Islander, yet very few Aboriginal boys were circumcised at such a young age. Aboriginal boys were most likely to be circumcised between 10 and 14 years of age. Other regional variations may also be reflected in the circumcision rate; for example, the higher circumcision rate in the Great Southern region may be influenced by a strong Muslim presence in some local communities. However, <1% of the Western Australian population was Jewish or Muslim according to 1996 Census data (Australian Bureau of Statistics) and religious circumcisions were not considered to impact significantly on the high routine circumcision rates of boys <6 months of age.
This difference between country and metropolitan medical practice has also been observed with other medical procedures in Western Australia. Rates of appendectomy, for example, are higher in country areas compared with metropolitan Perth.26 Thus, the different rates of routine circumcision between country and metropolitan areas may be due to more pervasive reasons common to all medical practice in Western Australia. The sometimes marginal economic viability of country medical practice may provide a perverse financial incentive for elevated elective procedure rates. There could also be less peer pressure for country physicians to adopt changing medical practice guidelines compared with physicians in metropolitan areas. Such issues need to be identified and addressed to ensure that country regions are not being disadvantaged in the provision of health care.
In contrast to boys <6 months of age, the rate of circumcision in boys 6 months and older but <15 years significantly increased over the 19 year study period. This increase was observed in non-Aboriginal boys. This suggests that some parents, in line with medical recommendations, may have delayed routine circumcision until their sons were older than 6 months. However, the lower overall circumcision rates in these boys was likely to be susceptible to other subtle changes in the cultural and religious environment in Western Australia during the study period. Muslims, for example, commonly practice circumcision, although unlike Judaism there is variation in the age it is performed, ranging from at birth and when aged 3-7 years of age.2 Thus, the increased rates of circumcision of boys aged 3-7 years of age may be a reflection of the Muslim population that increased from 0.25% in 1981 to 1.1% of the Western Australian population in 2001 (Australian Bureau of Statistics).
The cost of routine circumcision to the health-care system is considerable. Approximately 1500 unnecessary circumcisions are performed each year in Western Australia. This equates to approximately 15 000 circumcisions per year Australia-wide. Costs are estimated to range from $100 to $1600 for each circumcision, depending on whether hospital admission and general anaesthesia are involved. Therefore, Medicare, the national insurance system, spends somewhere between $1.5 and $24 million per year on a procedure deemed unnecessary by the Australasian Association of Paediatric Surgeons. The potential savings to the public purse would be considerable if elective and discretionary circumcision was removed from the Medicare schedule in line with other cosmetic surgeries, leaving rebates for the genuine medically indicated circumcision.
Removing the rebate may also encourage parents to reconsider having their young sons circumcised. The main reasons that parents gave for circumcising their sons 35 years ago was a desire to conform to the Australian norm, uniformity with father or siblings, and hygiene.27 Given that the uncircumcised state has become the norm today, further research is required to establish whether it is for hygienic, prophylactic or aesthetic reasons that some parents continue to circumcise their newborn sons in Western Australia. Identifying the reasons will inform the best approach to educating parents about the current medical opinion, which does not support routine neonatal circumcision. Education could be further targeted towards the parents of middle class socioeconomic status, who were found in the present study to be more likely to have their sons circumcised.
In comparison with other countries the rate of routine circumcision of boys <6 months of age in Western Australia is less than that reported in the USA and Canada, but higher than rates reported in New Zealand and England. The declining trends in Western Australia are consistent with the international and national medical practice guidelines that do not support routine circumcision, although there remains room for further reductions in the procedure, particularly in country areas. While circumcision will continue for reasons of religion or rite of passage in some cultures, these cases make up only a small number of routine circumcisions in Western Australia, particularly those performed on boys <6 months of age.
The authors thank the Data Linkage Unit, Western Australian Department of Health for the linked hospital morbidity data files. This project was funded through the Western Australian Safety and Quality of Surgical Care Project by a National Health and Medical Research Council research grant.
K. Spilsbury PhD; J. B. Semmens MSc, PhD; Z. S. Wisniewski MB BS, FRACS; C. D. J. Holman MB BS, PhD.
Correspondence: Dr J. Semmens, Western Australian Safety and Quality of Surgical Care Project, Centre for Health Services Research, School of Population Health, University of Western Australia, 35 Stirling Highway, Crawley, WA 6009, Australia.
Email: james.semmens@uwa.edu.au
Accepted for publication 23 January 2003.
The Circumcision Information and Resource Pages are a not-for-profit educational resource and library. IntactiWiki hosts this website but is not responsible for the content of this site. CIRP makes documents available without charge, for informational purposes only. The contents of this site are not intended to replace the professional medical or legal advice of a licensed practitioner.
© CIRP.org 1996-2024 | Please visit our sponsor and host: IntactiWiki.