Journal of Urology, Volume 144, Pages 1203-1205. November 1990.
Department of Surgery, Division of Urology, UCLA School of Medicine, Los Angeles and
Sepulveda Veterans Administration Medical Center, Sepulveda California
Journal of Urology, Volume 144, Pages 1203-1205. November 1990.
Department of Surgery, Division of Urology, UCLA School of Medicine, Los Angeles and
Sepulveda Veterans Administration Medical Center, Sepulveda California
A simple technique is described for plastic reconstruction of the prepuce. Penile skin is used and the defect created is covered by implantation of the penis into the scrotum. At a second stage the penis is released from the scrotum. (J. Urol., 144: 1203-1205, 1990)
Since the topic of circumcision continues to be controversial, the present status has been neatly summarized by Hinman1 as well as others, including the American Academy of Pediatrics Task Force on Circumcision.2,3 However, there is a small group of circumcised men who would like to regain a prepuce. A simple reliable operation is described for reconstruction of a foreskin. Penile skin is used to reproduce a prepuce after circumcision. Anterior scrotal skin, which by its elastic nature, coloring and appearance is an ideal substitute for needed extra penile skin, is used as a readily available in situ skin graft.
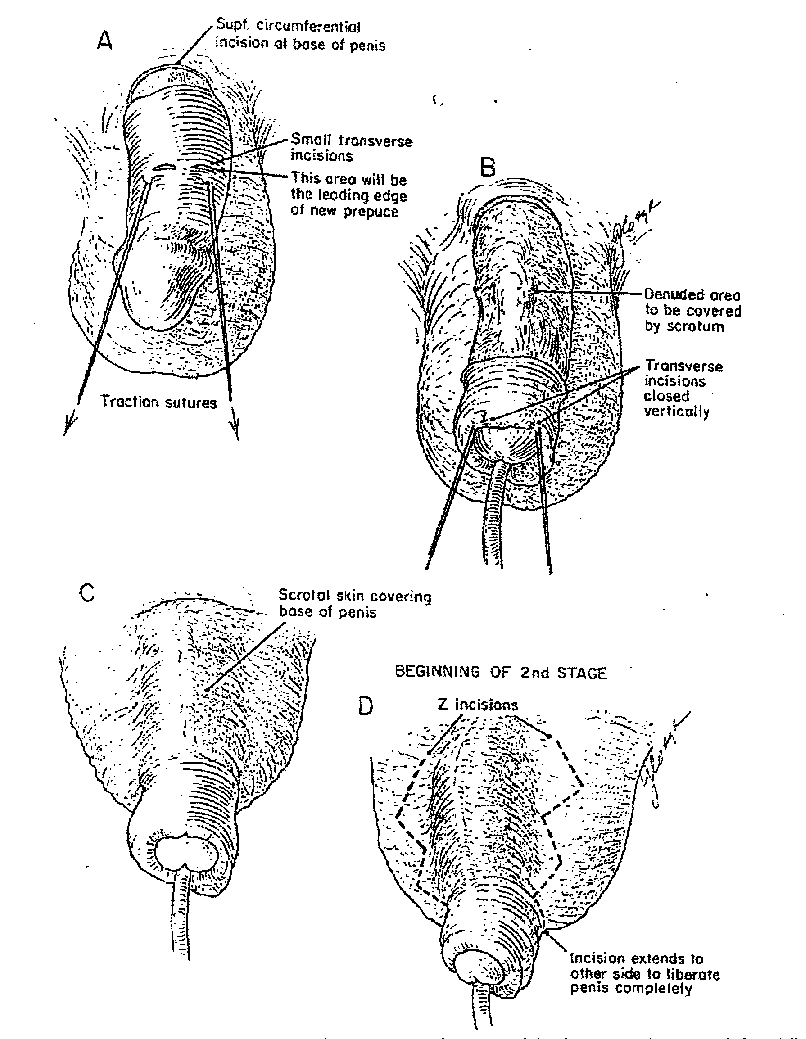
The distal penile skin is mobilized is such a way as to be pulled down in a double layer to form a new prepuce. This is done by making a superficial circumferential incision around the base of the penis (part A of figure). The incision should not be so deep as to destroy important blood supply. The distal portion of the penile skin to be used for the new prepuce is identified. Stay sutures are placed to pull the skin down to cover the glans (part B of figure). Once these relationships are established 3 or 4 small transverse incisions are made in what wil be the leading edge of the new foreskin. Then by careful dissection with scissors the entire skin around the head of the penis up to the glans is mobilized. Further mobilization of the skin is done by blunt scissor dissection in the immediate subcutaneous area on the proximal portion of the penis.
This allows the distal penile skin, including the the remaining mucosal type of skin, to be pulled downward over the head of the penis. The transverse incisions are closed in a vertical fashion, thus narrowing the circumference of the new prepuce, which has become like a small hood covering the glans. Traction sutures should be placed on each side to ensure post operative tension and keep this new double layer approximated during the immediate postoperative period while the 2 inner layers grow together (part B of figure).
This procedure leaves a defect of skin at the base of the penis. This denuded area is covered easily with scrotal skin. Two transverse incisions are made in the anterior scrotum and a shallow tunnel is created close to the scrotal skin between the two incisions. The penis then is pulled under the scrotal bridge and the skin edges are anastomosed. This method leaves the base of the penis buried in the scrotum (part C of figure) where the scrotal skin covers the denuded area.4 A catheter should be used and traction or adhesive binding to fix the new prepuce downward over the glans must be used for 5 or 6 days postoperatively.
After approximately 3 months stage 2 is accomplished by lifting the penis out of the scrotum as described previously.5 It is noteworthy that at stage 2 incisions should be made in a Z form on each side to provide plenty of scrotal skin for closure of on the ventral side of penis. This method prevents a vertical scar (Part D of figure).
The procedure is remarkably simple. Patients do experience significant edema and postoperative discomfort, and attention mut be directed to prevention of erections until the distal skin has grown together. Rubin6 described a similar operation by Penn who used a skin graft instead of scrotum to cover the defect.7 The scrotum is an adjacent graft with good blood supply, and it appears much more normal and accommodating than a skin graft from elsewhere on the body.
The idea for this technique originated from reconstruction of penile skin4 and experience with phalloplasty.5 Later it was learned that the method is a modification of an ancient operation described by Celsus, who wrote during the reign of Tiberius in AD 14 to 37. He described 2 such operations. Apparently, it was not then infrequent to undergo the operation for he patient to move inconspiciously in Greek and Roman society.
Anyone wishing to understand this historical note further (although this operation may seem to be strange in our times) should refer to the history as reported by Rubin, who described problems of ancient times, especially as they concerned Jews and gladiators.6 This classical article not only is well referenced but well illustrated to show the technique used in those times. The operation described in the current article is similar but, since it is done in two stages, it may be somewhat less brutal.
Further notes on historical aspects of this problem are presented in the chapter on history of external genital surgery by Rogers.9 Writing of Roman medicine and surgery, he stated:
Psychiatric considerations are considerable and have been reviewed by Mohl and associates.8
There are other methods to perform this operation. Some patients have elongated the penile skin by long-term traction, using adhesive tapes to pull the skin down and keep it tight over the glans. In Roman times this was done by what they called infibulation,
in which a fibula was placed across the distal preputial skin and traction was applied.
One patient presented with a dorsal slit because of an acute infection during childhood. All of the normal preputial skin was still present and the patient wished the skin restored to a normal appearance. An inverted V-shaped incision was made where the dorsal slit had been and the two edges were sutured together, thus, reproducing the normal prepuce. The patient was delighted with the results. It could be that this might be an answer to some critics of circumcision. A simple dorsal slit can be performed in patients who have phimosis or severe recurrent infections. At a later date, if they wished restoration, reconstruction to the uncircumcised appearance would be simple.
One patient had successfully used traction and stretching
for a long period, which produced a nearly normal-appearing prepuce even though he had been circumcised. Possibly, the same result could be obtained by using 1 of the inflatable expanding devices that plastic surgeons currently are using to obtain extra skin. This could be a good means to expand area that is to become the new prepuce. Skin can, indeed be stretched. Of course, penile and scrotal skin is especially notable for elasticity. All men who experience erections are aware of this elasticity and accommodation to natural pressures.
Accepted for publication May 16, 1990.
The Circumcision Information and Resource Pages are a not-for-profit educational resource and library. IntactiWiki hosts this website but is not responsible for the content of this site. CIRP makes documents available without charge, for informational purposes only. The contents of this site are not intended to replace the professional medical or legal advice of a licensed practitioner.
© CIRP.org 1996-2025 | Filetree | Please visit our sponsor and host:
IntactiWiki.